Most conversations about immunity focus on supplements, detox, or inflammation. But one of the most important regulators of immune function is a small gland behind the sternum that most people have never heard of: the thymus.
The thymus trains and produces T-cells — the specialized immune cells responsible for identifying viruses, fighting infections, preventing autoimmune reactions, and surveilling for cancer. Without a functioning thymus, the immune system loses its ability to adapt to new threats. At Santa Maria Health, we increasingly see thymus-related immune decline as a central factor in patients presenting with chronic fatigue, post-viral conditions, and persistent inflammation.
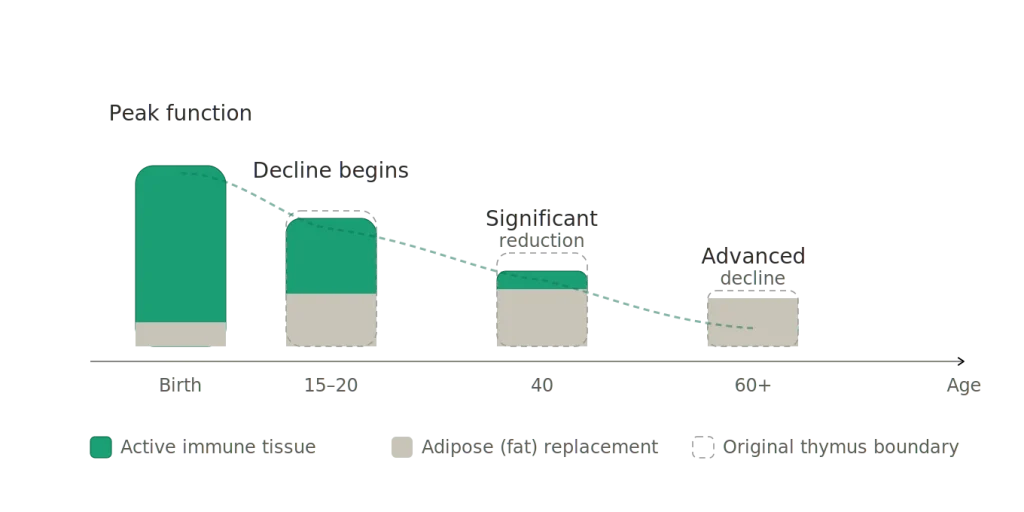
What makes the thymus unusual is that it begins to shrink early. Unlike most organs, which maintain their function well into middle age, the thymus starts involuting — replacing active immune tissue with fat — as early as the late teens. By age 40, thymic output is significantly reduced. By 60, the organ is largely adipose tissue. This process, called thymic involution, is one of the most consistent and consequential features of biological aging.
What Thymic Decline Actually Means for Health
The downstream effects of a shrinking thymus are broad and clinically significant. As the thymus involutes, the body produces fewer naïve T-cells — the immune cells capable of recognizing new pathogens. The result is a progressive narrowing of the T-cell repertoire: the immune system becomes increasingly reliant on memory cells from past infections, and less capable of mounting effective responses to novel threats.
This decline is associated with:
- Increased susceptibility to infections, including respiratory viruses and reactivation of latent viruses such as Epstein-Barr
- Reduced cancer surveillance — the immune system’s ability to detect and eliminate abnormal cells
- Higher rates of autoimmune dysregulation, as thymic selection of self-tolerant T-cells diminishes
- Slower recovery from illness, surgery, or injury
- Chronic low-grade inflammation (sometimes called “inflammaging”), driven by an aging immune system compensating for lost adaptive capacity
For patients who describe feeling like their body “can’t fully recover” — from a virus, from fatigue, from persistent inflammation — thymic decline is often part of the underlying picture.
New Science: Can the Thymus Be Supported or Restored?
Until recently, thymic involution was considered an irreversible feature of aging. That view is shifting. Several lines of research from 2019–2025 now suggest that thymic function can be partially preserved or even restored.
The TRIIM Trial (Fahy et al., 2019)
The most widely cited result comes from the TRIIM trial (Thymus Regeneration, Immunorestoration, and Insulin Mitigation), published in Aging Cell in 2019. In this small pilot study of 9 healthy men aged 51–65, a combination of growth hormone, DHEA, and metformin was administered over 12 months. MRI imaging showed regeneration of thymic tissue, increased naïve T-cell counts, and — unexpectedly — a reversal of epigenetic aging by approximately 2.5 years as measured by multiple epigenetic clocks, including GrimAge.
Important context: this was a very small, uncontrolled study. The results are intriguing but preliminary. A larger follow-up trial, TRIIM-X (NCT04375657), enrolling 80–100 men and women aged 40–80, is currently underway through Intervene Immune.
FGF21 and Metabolic Regulation of Thymic Aging
A 2025 study published in Nature Aging (Wedemeyer et al.) demonstrated that FGF21 — a metabolic hormone linked to caloric restriction and longevity — plays a direct role in maintaining thymic function. In mouse models, locally produced FGF21 in thymic stromal cells regulated mTOR signaling in nearby epithelial cells, preserved thymic architecture, and maintained a broader T-cell repertoire with age. A companion study by Youm et al. showed that elevating FGF21 delayed thymic involution and extended healthspan.
The practical implication: thymic aging is not purely a clock running down. It is metabolically regulated, and interventions targeting metabolic pathways — including caloric restriction, which induces FGF21 — may have direct thymus-preserving effects.
The System Behind the Thymus
Focusing on the thymus alone is not enough. Thymic function is deeply integrated with metabolic health, hormonal balance, sleep quality, chronic infection status, and inflammation levels. Standard medicine treats the consequences of immune decline without addressing the systemic environment that drives it. Functional medicine clinics often engage with metabolic and hormonal layers but without biomarker-guided evaluation of immune function itself.
The emerging science points toward a systems-level strategy: reducing the chronic inflammation that accelerates thymic involution, restoring metabolic signals (including pathways like FGF21) that support thymic maintenance, optimizing sleep and circadian rhythms, and addressing hormonal imbalances that directly influence immune cell production.
Our Approach at Santa Maria Health
At Santa Maria Health, we approach immune health as a systems problem. Rather than targeting the thymus directly — no validated clinical intervention exists for that yet — we focus on restoring the biological environment that supports immune resilience and, by extension, thymic function.
Our diagnostic programs evaluate metabolic health, inflammatory markers, hormonal balance, and immune status as an integrated picture. Treatment programs are designed around the individual patient’s profile: reducing chronic inflammation through targeted therapies and detox pathways, restoring mitochondrial and metabolic function, optimizing sleep architecture, and addressing hidden infections or immune dysregulation.
This approach reflects the direction the science is pointing: immune aging is not a single-organ problem, and the most promising interventions work at the level of the system, not the symptom.
For patients experiencing chronic fatigue, post-viral conditions, persistent inflammation, or simply a sense that their body is no longer recovering the way it used to — understanding thymic function and the system that supports it can be the missing piece. Learn more about our Health Programs or explore our approach to regenerative medicine.